Most People Don’t Know They’re Becoming Insulin Resistant — Until It’s Too Late
There’s a common assumption in healthcare:
If your blood sugar is “normal,” you’re metabolically healthy.
But that assumption is often wrong.
Long before blood sugar rises, long before a diagnosis is made, and long before symptoms become obvious — the body is already changing.
Insulin sensitivity is one of the earliest places those changes begin.
And for many people, it’s declining silently.
What Insulin Sensitivity Really Means (And Why It Matters)
Insulin is the hormone that helps your body move glucose out of your bloodstream and into your cells, where it’s used for energy.
When your body is insulin sensitive, this process works efficiently:
- You maintain stable energy
- You recover well from meals
- You avoid excess fat storage
- Your metabolism stays flexible
But when insulin sensitivity begins to decline, the body compensates.
It produces more insulin to achieve the same effect.
And that’s where the problem starts.
Insulin resistance doesn’t begin with disease.
It begins with inefficiency.
The Silent Shift Most People Miss
Here’s the issue:
This process doesn’t happen overnight.
It unfolds gradually — often over years — and usually within “normal” lab ranges.
You might notice subtle signs:
- energy crashes after meals
- increased hunger or cravings
- difficulty losing weight
- stubborn abdominal fat
- poor recovery or sleep
Individually, these feel manageable.
Collectively, they point to something deeper:
your metabolism is becoming less efficient.
Why Traditional Healthcare Misses This
Most healthcare systems are designed to detect disease — not early dysfunction.
That means:
- Blood sugar has to rise significantly before concern is triggered
- Insulin is often not measured at all
- Trends over time are rarely tracked
By the time intervention happens, the system has already been under strain for years.
At EverSpan Life, we take a different approach.
Health doesn’t change suddenly.
It shifts gradually — and those shifts can be measured.
What Happens If You Ignore It
As insulin sensitivity declines, the body becomes more likely to:
- store excess energy as fat
- increase systemic inflammation
- disrupt lipid metabolism
- impair recovery and energy production
Over time, this increases the risk of:
- metabolic syndrome
- type 2 diabetes
- cardiovascular disease
- fatty liver disease
- cognitive decline
But more importantly — it changes how you feel long before those diagnoses.
Less energy.
Less resilience.
Less capacity.
The Part Most People Get Wrong About “Fixing It”
Most advice focuses on surface-level solutions:
- “eat better”
- “exercise more”
- “reduce sugar”
These matter — but they’re incomplete.
Because without understanding your specific biology, you’re guessing.
And guessing leads to inconsistent results.
How to Actually Improve Insulin Sensitivity
Improving insulin sensitivity is not about one tactic — it’s about aligning multiple systems.
1. Nutrition That Stabilizes, Not Spikes
Meals built around protein, fiber, and healthy fats help regulate glucose and reduce insulin demand.
2. Muscle as a Metabolic Lever
Resistance training increases your body’s ability to absorb and utilize glucose. Muscle is one of the most powerful tools for metabolic health.
3. Movement After Meals
Even a short walk can significantly improve glucose handling.
4. Sleep and Circadian Alignment
Poor sleep and disrupted rhythms directly impair insulin signaling — something most people underestimate.
5. Stress Regulation
Chronic cortisol elevation can drive insulin resistance even in otherwise “healthy” individuals.
Why Biomarker Testing Changes Everything
Here’s where most people finally gain clarity.
At EverSpan Life, we don’t just look at glucose.
We analyze a broader metabolic picture, including:
- fasting insulin
- glucose trends
- inflammatory markers
- lipid patterns
- hormone interactions
Because what matters isn’t just your current number.
It’s the direction your biology is moving.
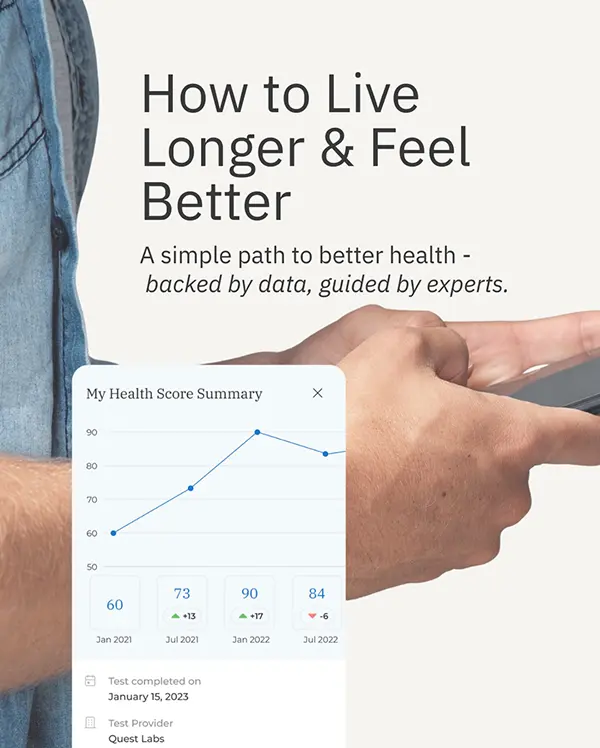
Tracking these markers over time allows us to:
- identify early metabolic shifts
- personalize interventions
- adjust strategies based on real data
- prevent decline instead of reacting to it
The Real Goal: Metabolic Flexibility
The goal isn’t just “normal labs.”
It’s metabolic flexibility — the ability to:
- efficiently use energy
- switch between fuel sources
- recover quickly
- maintain stable performance
This is what allows you to:
- feel energized throughout the day
- maintain a healthy body composition
- support long-term brain and cardiovascular health
- age with strength and resilience
The Bottom Line
Most people think insulin resistance starts when they’re diagnosed.
In reality, it starts years earlier — quietly, gradually, and often invisibly.
The good news is:
That means you have time.
Time to measure.
Time to adjust.
Time to improve your trajectory.
Because the goal isn’t just to avoid disease.
It’s to maintain the energy, clarity, and capability that make life worth living.